Platelet Rich Plasma
Platelet Rich Plasma – Another Tool in Regenerative Medicine
The underlying principle is simple – injections of high concentration of platelets to stimulate healing of a chronic or acute non-healing injury.
Use of the patient’s own blood (autologous blood) to obtain the platelets helps eliminate the risk of disease transmission or allergic reactions.
Composition of blood:
- Platelets: Blood contains less than 1% platelets. Platelets are produced in the bone marrow and have an average life span of 7-10 days from the time they are produced. The function of platelets is hemostasis i.e. it stops bleeding. However, platelets also stimulate formation of new blood vessels and form new connective tissue.
- Red cells: Blood contains about 44% red cells which deliver oxygen from the lungs to the other cells.
- White cells: White cells constitute about 0.7% of blood. They fight infections, kill germs and carry off dead red cells. For every 600 red cells, there are 40 platelets and 1 white cell.
- Plasma: the liquid part of blood constitutes about 54.3% of blood. It is made mostly of water and helps to transports cells in the body. Plasma also contains fibrinogen, a protein that acts like a net and catches platelets at a wound site to form a clot.
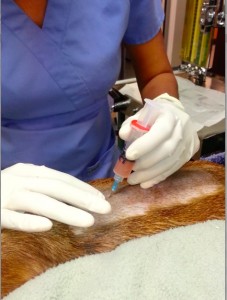 In PRP therapy, we decrease the red cell concentration to 0-5% and increase the platelet concentration to 94%. Why? This is because red cells are less useful in the healing process while platelets are highly beneficial.
In PRP therapy, we decrease the red cell concentration to 0-5% and increase the platelet concentration to 94%. Why? This is because red cells are less useful in the healing process while platelets are highly beneficial.
So, let us get to know our friends the platelets better, shall we? They are tiny cells in the blood, way smaller than the red cells and they contain many small granules. These little granules secrete beneficial substances called growth factors.
When a platelet is activated by inflammation and injury, it releases these growth factors which attach to neighbouring cells. This stimulates the local cells to form more of the same cells (cell proliferation) or differentiate into other cells (cell differentiation) and also repair injured tissue. Just imagine, within one hour of injection, 95% of these growth factors are secreted!
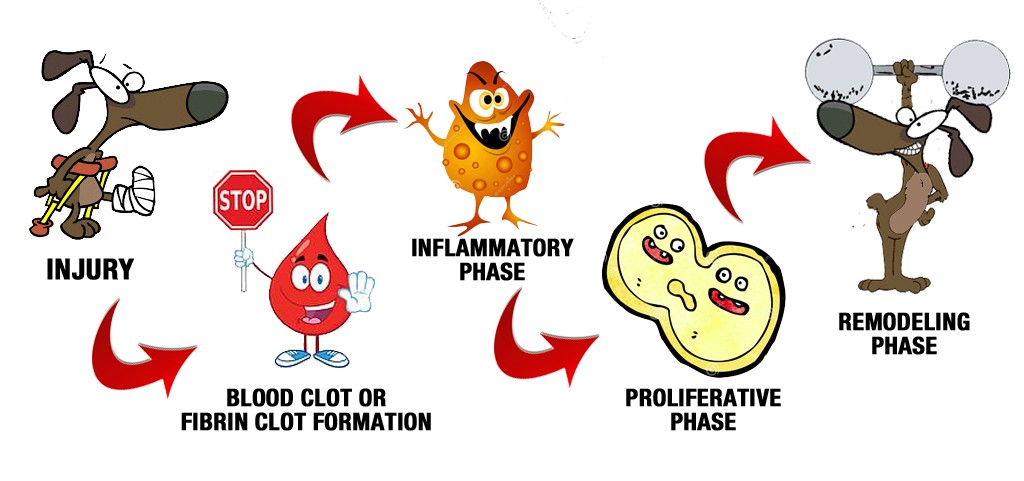
To understand what happens when we inject platelets, we should know the sequence of events following an injury.
When an injury occurs there is some bleeding internally or externally. The platelets tend to collect at the site to form a clot. This is the inflammatory phase and can last 1-3 days. Inflammation is characterized by redness, swelling and pain – the sequence of events we are all familiar with following an injury. All this happens because of the release of growth factors from the platelets enmeshed in the clot.
The next phase known as the proliferative phase can last for weeks. At this time, the growth factors attach to cells and these cells produce or differentiate into new cells and new blood vessels are formed.
The last phase of injury is the remodelling phase. This is the final stage of healing response following an injury where the newly formed tissue matures and strengthens.
When is PRP used?
I use PRP to treat torn cruciate ligaments, hip dysplasia, elbow dysplasia, patellar luxations, osteo-arthritis of any joint and for intervertebral disk disease causing severe back pain and neck pain in dogs and cats. The elbow joint is my least favourite – this is a very unforgiving joint as there is very little space between the bones and healing is prolonged. Compared to a 95% success rate with other joints, my success rate with elbow joints is considerably lower. And yet, if I can give the elbows a chance to heal, I will still do it. In the future, I hope to try multiple treatments of prolotherapy in the elbow joint (once weekly over 4 weeks) to see if I can achieve better results on these patients.
How does it help?
 Ligaments and tendons are strands of dense fibrous tissue resembling ropes and are involved in the stability of the joint. The greatest amount of stress to ligaments and tendons is where they attach to bone. In the interest of embracing rather than suppressing the inflammation, PRP injections prompt a local inflammation. This triggers a wound healing cascade, and results in the deposition of new collagen. Collagen is the tissue of which tendons and ligaments are composed. The new collagen contracts as it matures, in turn tightening and subsequently reinforcing the injected painful area. That is all the body requires, the remaining healing stages take care of themselves.
Ligaments and tendons are strands of dense fibrous tissue resembling ropes and are involved in the stability of the joint. The greatest amount of stress to ligaments and tendons is where they attach to bone. In the interest of embracing rather than suppressing the inflammation, PRP injections prompt a local inflammation. This triggers a wound healing cascade, and results in the deposition of new collagen. Collagen is the tissue of which tendons and ligaments are composed. The new collagen contracts as it matures, in turn tightening and subsequently reinforcing the injected painful area. That is all the body requires, the remaining healing stages take care of themselves.
Tendons and ligaments have limited blood supply which is why they heal poorly following injury. Next to the periosteum, the outer lining of the bone, these structures are also the most painful. PRP helps alleviate pain as well as rebuild new tissues.
 About 15 ml of blood is drawn from the patient into a PRP syringe prior to sedation. Some dogs and cats do not tolerate even this minor procedure and may require sedation prior to blood draw. As this lowers the blood pressure and causes the blood to clot while it is being drawn, I add some anti-coagulant to the syringe in these cases.
About 15 ml of blood is drawn from the patient into a PRP syringe prior to sedation. Some dogs and cats do not tolerate even this minor procedure and may require sedation prior to blood draw. As this lowers the blood pressure and causes the blood to clot while it is being drawn, I add some anti-coagulant to the syringe in these cases.
The blood is spun down in a PRP centrifuge for 10 minutes. The top layer of PRP is drawn out and kept ready for injection. For multiple joints, I sometimes have to use 2 syringes.
The hair over the affected area or joint is clipped and the area prepped with antiseptics so that the PRP can be drawn out and injected ensuring complete sterility.
Depending on the patient’s pain tolerance, sedation may be required. I prefer to sedate for a brief period of 10-20 minutes so that the injections can be done quickly and efficiently with minimal trauma to the patient. I also reverse the sedation after the procedure and my patients are able to walk out of the clinic within 10 minutes usually. I have performed the procedure on some patients with acupuncture sedation alone, however responses can vary between patients and use of injections is often necessary to achieve sedation.
A hand-out is provided at the time of scheduling an appointment with instructions regarding withdrawal of anti-inflammatories, preparation for the procedure and rehabilitation guidelines after the procedure.
What happens after PRP?
After the procedure, I usually prescribe specific guidelines every 2-4 weeks regarding duration of walks, passive range of motion and weight-bearing exercises. I strongly recommend and refer patients for underwater treadmill and controlled swimming which facilitates good healing and faster recovery. The reason is that buoyancy and the resistance of water both play a role in encouraging the patient to bear weight on the affected limb as well as learn to move the limb through a more natural range of motion. This literally resets the nervous system and the musculo-skeletal system and the patient learns to use the limb again without fear of pain.
I am currently collaborating with an orthotist to design custom braces for patients that undergo PRP or prolotherapy treatments. Use of braces to provide support and correct the angle of the joint is crucial to recovery. Conformation varies between different breeds of dogs and cats and even between individuals. Therefore, I find customized braces provide better
Contra-indications to PRP
The one contraindication is neoplasia which is cancer. IF there is the slightest suspicion of cancer, I refrain from performing this procedure. This is why I do not perform the procedure without reviewing recent x-rays and sometimes, even seek a radiologist’s opinion for suspicious lesions on the x-ray.
I refer some patients for surgery based on breed, weight and severity of pain. However, PRP treatments do not necessarily preclude surgery and patients can still go through surgery in cases of re-injury or if they do not heal.